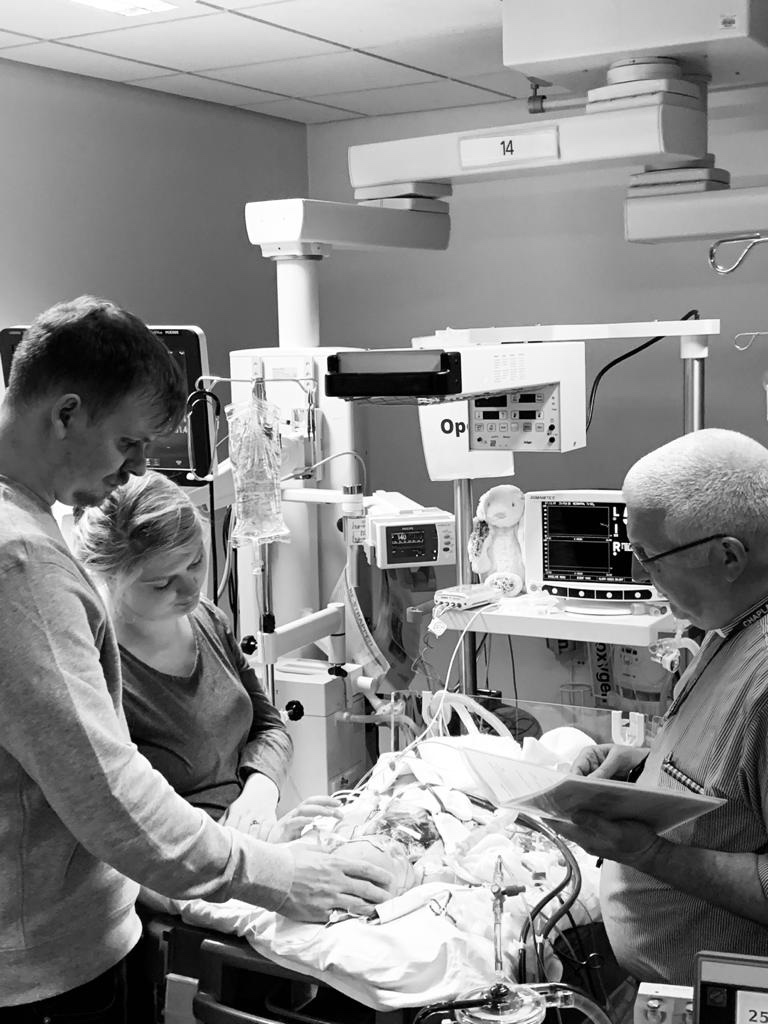
I’m publishing this blog post now after my baby boy is safely here but I tried to write down my thoughts and feelings as and when I felt them while pregnant. It feels strange to read it back because it already feels like a lifetime ago. I wasn’t sure whether to post it but I’m doing so in case it resonates with others going through it or if they are wanting to support somebody who is.
What did I expect to feel when pregnant after loss? I expected to feel joy for new life, hope I would bring this baby home and a lot of fear and anxiety that I wouldn’t. Turns out there were a lot of other feelings in between. I’ll be honest- it’s not a cheery read but I think it’s important to acknowledge the challenges that so many go through.
A friend described pregnancy after loss as the second hardest thing they ever went through and I understand that now. Physically and mentally- it’s a test of endurance. For those who have seen me this pregnancy, some of these words might come as a surprise, as outwardly I think I may seem to have had it all together. I coped the best that I could but these last few months have served as a reminder that others may be facing real heartache undetected by others too. You should always ask if somebody is OK twice!
Here is my pregnancy stream of consciousness…
The First Trimester
I’m very twingey. Every twinge is nerve-wracking. Every trip to the toilet is a check for blood. I panic about bleeding in public places and consider whether I should start wearing pads just in case. I wear one for my job interview because that feels like an awful thing that could happen- to begin bleeding in a stressful situation in front of strangers.
I cry when I have to repeat what happened with Etta to different health professionals. It feels strange to see it written in my maternity notes that this is my 5th pregnancy- and that my last 2 were delivered at home. They were not the home birth that I hoped for.
I also cry (and Sam does too 🤭) when we hear baby’s heartbeat at our private scan. I am 8+5 weeks pregnant. We haven’t had good news on a scan for a long time. We let ourselves be happy and excited and tell our family as it feels a little more likely that this baby will be sticking around. But I know that I hadn’t miscarried Bumblebee by this point yet so still feels like I need to hold my breath.
With every week that passes I feel both more hopeful and more fearful. I know my chance of miscarriage is lowered but also I don’t want to miscarry a fig or a lime- an olive was traumatic enough. The fruit/veg size of my baby used to be a lovely thing to look at but now it feels like a terrifying warning.
I don’t like it when people congratulate me because it doesn’t feel like pregnancy is something to celebrate anymore. Bringing home a healthy baby is. And sadly, my experience is that babies are more likely to die or pregnancies are more likely to end than continue.
Being told to ‘stay positive’ is annoying as it will not change the outcome. And I don’t think being negative causes you to miscarry. I’m going to try and let hope creep in where it can but telling someone to be positive is always annoying.

Did statistics used to be comforting? I don’t know but now I think the percentages are actually terrifying. Maybe because we’ve been on the wrong side of those statistics a lot of times now. (I know logically that neonatal deaths and miscarriages after 8 weeks are rare).But suddenly 1 in 250 babies being stillborn feels like a lot. We have a 3% chance of this baby having a heart defect. 1 in 33 doesn’t feel great. Especially considering about 1 in 40 babies are born with any birth defect too. We were told that Etta’s survival rate for her first surgery was 85-90%. How can you apply statistics like that to the reality of your child dying? But she did survive- and got through the riskiest part to then rapidly decline when nobody expected it and no statistics had been offered.
4 friends/family are due in the Summer. I’m so excited for them. I’m so anxious for them. I have to apologise for my ‘scanxiety’ and ask them how it’s gone because otherwise I’ll be panicking for ages. I try really hard not to show anything except joy but it can be exhausting. It’s not their fault that my baby died but I know it makes this wonderful news more complicated. I know one of my grief triggers is hearing someone is in labour so I will probably try and avoid that and wait for a happy announcement instead.
I have the IAPT (NHS talking therapy service) website open on my phone. I keep thinking about calling them. But I know the waiting list will be long and by the time I’ve got an appointment what I wanted to talk about is probably irrelevant. At the moment it’s enough to know it is there.
This week, I’m flitting between ignoring I’m pregnant and then devouring entire forums with other women due at the same time. I don’t really know what that’s about- maybe I’m trying to get used to the idea.
I’ve thought about names. Stressed about how to get a nod to Etta in if it’s a girl. I would feel very happy at this point if baby was a boy or girl as long as they were healthy. I would love for Ezzie to have a little brother. I would love for Sam to have another chance at ‘daddy’s little girl’. It’s a win win.
I think this will probably be my last pregnancy so trying to appreciate it. I’m trying to not feel guilty when I don’t.
The Dating Scan- I thought I was going to have a panic attack in the waiting room. Luckily Sam could come into the scan room with me but had to wait outside the building until we were called in. The scan went smoothly- I still googled all the measurements after the scan. I’m not sure that part will ever leave me now in pregnancy. Etta is in my notes and they’ve even put a bright green sticker on the front of my notes to indicate a neonatal loss but the sonographer still didn’t know we had lost a baby (cue awkward conversations). On the plus side we didn’t have to pay for our pictures. Sympathy pictures like with Etta. I was warned this would happen but I’m still not looking forward to going over our story every appointment.
The Second Trimester

The anxiety had eased for a few weeks and I’m seeing a counsellor now which has helped with those feelings of overwhelm.
I hit 17 weeks pregnant a few days ago and it just feels like a very anxious countdown to our 20 week scan. The 20 week scan is massive- we are only slightly more likely to have a baby with a heart defect but it still feels like a big chance to us. Sam and I keep panicking that they might have a birth defect which isn’t a heart thing- we know hearts now but what if they have a problem with their kidneys?!
Distraction is the only way to keep going.
The Anomaly scan- the day finally arrived and the consultant was great- talked through our history. Referred to Ezzie and Etta by name throughout and explained everything as he went along. It was strange looking at a healthy heart but we could see it there clearly along with another clear bit of anatomy that told us we were expecting another little boy.

Immediately there was an adrenaline dump and we just felt pure relief, happiness and exhaustion. But I think it slowly sunk in that we weren’t having another girl and also that we weren’t getting another chance with Etta. Of course I knew rationally that this baby couldn’t be Etta but I’m not sure that I really processed that. I remember at the beginning of the pregnancy hoping this child would have a heart defect so that we would get to experience being heart parents where we actually get to live out the reality of years of hospital appointments and worry- it’s what we had prepared ourselves for. It sounds stupid because obviously I don’t want that really- I want a healthy child.
And that night of the scan, after being up with Ezzie, I cried a lot to Sam. I felt guilty for wanting this baby to be Etta when this baby boy is also wanted. I want both of them. And I want a chance to be pregnant with Etta and do it all again but this time she doesn’t die and we live happily ever after. Life feels especially cruel today. I know Sam feels it too- the fact that this baby looks healthy emphasises how unfair it is that Etta wasn’t.
The weekend after our 20 week scan was hard. I just felt really sad. I’ve tried to be honest when people say how happy and excited they are for us. It can feel a lot of pressure. I’ve just tried to go with ‘we are very excited and relieved but…’ I think it’s important to try and explain some of the negative feelings otherwise I’ll feel the need to put a brave face on throughout the whole pregnancy and that won’t help anyone!
A few weeks on from the 20 week scan and I feel the calmest I’ve felt so far. My anxiety is low at the moment and I sometimes get excited about this baby too. I’m trying to look at things for the nursery and baby clothes but it still feels a bit ‘fake it til you make it’ at the moment. Every happy feeling then just makes me feel sad.

My counsellor explained that when you lose someone you love you are triggered by anniversaries, special places and memories of them but when you’re pregnant after the loss of a baby you are basically living one big trigger constantly. It helped me a little bit to understand why pregnancy after loss can be so exhausting and so sad. Every movement in my tummy takes me back to being pregnant with Etta. Preparing for this baby’s arrival reminds me of all the things we did to prepare Ezzie and our home for Etta. It is just so bittersweet all the time.
Grief is exhausting but you carry on. And this little miracle is so loved already.
Fathers Day felt hard this year. And of course I felt guilty for being griefy on this day which should really be all about Sam’s feelings. But I couldn’t shake the feeling that this time the year before I had bought a present from Ezzie, Etta and Bumblebee bump only to then start bleeding the following day. Needless to say, I put off buying a Father’s Day present until the last minute this year. It was hard not to associate the day with sadness but I was still so grateful to celebrate with my own dad and Sam. Maybe these days will always be a bit shit and hard now, along with Christmas, birthdays, family gatherings, holidays, days ending in y… etc etc.
The Third Trimester
I turned 28 weeks last week and it felt like another big milestone- entering the third trimester, where suddenly appointments pick up, more things can go wrong and it’s the final stretch before the due date.
I’ve started not sleeping very well again as a result of the anxiety. I’m so exhausted but then I get into bed and can’t switch off. I’m hoping that once I get to the Summer holidays, I’ll have less work stuff to think about but also know that I’ll be losing my best distraction.
I’ve been having horrible dreams about stillbirth and it’s hard to shake the graphic pictures in the morning. I feel like I’m constantly having flashbacks to our time in Bristol too- little memories pop up all the time. I’ve also been looking at photos a lot but I still find it hard to see the transformation of our gorgeous little newborn into such a poorly baby.
I’m planning a homebirth because I think I will struggle mentally to give birth in hospital. The smells, the sounds, the sights are hard to dissociate to our time in Bristol and to a lesser extent, scans and the miscarriage too. But of course, it comes with a little bit of anxiety- especially on Sam’s part!
They’ve said I’ll need an appointment at 34 weeks to discuss all the risks etc. (the same risks as in hospital but no emergency button at home) which I’m sure will be stressful! Unfortunately, you don’t have to be told adverse statistics when you give birth in hospital or a midwife unit but you do at home. However, I know it’s the right decision for this birth as it’s where I’ll feel safest. I didn’t get to bring Etta home but if I have this baby at home then at least they will be at home with us. Even if they die. Because of course they might still die and it’s hard not to caveat every hope and wish for this baby’s future with ‘if all goes well’, ‘if this baby survives’ or ‘if this baby is healthy’.

I think the experience of Etta dying just opens your eyes up to all the possible things that might go wrong and life after loss is like walking the tightrope of knowing that terrible things might be waiting right around the corner while holding onto hope that it won’t or that if it does you’ll still survive it. So of course this pregnancy has also been ravaged with thoughts of me getting cancer in a few years time, Ezzie getting cancer in a few years time and this baby dying shortly after birth because of something they couldn’t pick up in pregnancy. There’s no such thing as filling your grief or suffering quota. I wish there was! But I still think that if all the suffering was shared out across the whole world, then we would still have lucked out with our current lives. So it’s important not to lose the gratitude. Gratitude is everything as it turns out.
This evening we went in for reduced movements at 30 weeks pregnant. I actually feel proud that it’s taken me this long to have to go in. That sounds stupid because obviously I can’t control the baby’s movements but part of me thought I might need the reassurance of scans and monitoring constantly when actually I have managed without. This baby is so wriggly I’ve not had to worry at all. Until today. I don’t think Sam and I realised how anxious we were until we heard a heartbeat and we burst into tears. The midwife looked a bit confused so we tried to explain that we had lost babies before. (She later apologised when she’d had time to read our notes). Everyone was really kind and booked us in for a reassurance scan later on in the week.
And then finally it’s the final countdown before his arrival. I swing between knowing he will come when he is ready and also just wanting him to hurry up and get here!

His Arrival
And then on the 25th September at around 4 am in the morning our gorgeous Reuben came into the world. The delivery was scary and calm at the same time- like the weeks before his birth. When I realised that we would likely be delivering him at home without any medical professionals, I started to panic. What if he was born not breathing? What if he got stuck on his way out? Like many times in my motherhood journey, I really felt I had to dig deep to stay calm and trust that my body and baby knew what they were doing. I was lucky to have my mum and Sam on hand too.
Hearing his cry was pure relief. And when the midwife arrived only a few minutes later all I could ask was “Is he OK?” because that was all that mattered.

Like I wrote in my poem, pregnancy after loss is a test of endurance but I would do it again and again for each of my 3 babies. One of the affirmations I had up on my wall in labour was “Giving birth is the ultimate act of love” and I would argue so is the 9 months leading up to it. On the days I didn’t feel so courageous, it was my love for Reuben that carried me through. ❤️