*** Trigger Warning *** This post details the day of Etta’s cardiac arrest and photographs from that day so don’t read on if that will be a bit much for you ❤️
Yesterday was a really heavy day. I spent most of the day crying or on the verge of crying or with a headache from crying so much. There were a lot of tears. So I thought maybe writing about this day might help.

14th December 2019- I think of this day as when it all started going wrong and the beginning of the end. Etta’s death came as a shock to many because up until this point she had been recovering well from her surgery and we all very much thought the hardest and riskiest part was over. We would never see Etta awake again after this day, despite the huge amount of hope that we and her doctors had that she would pull through. So I will start at the beginning…
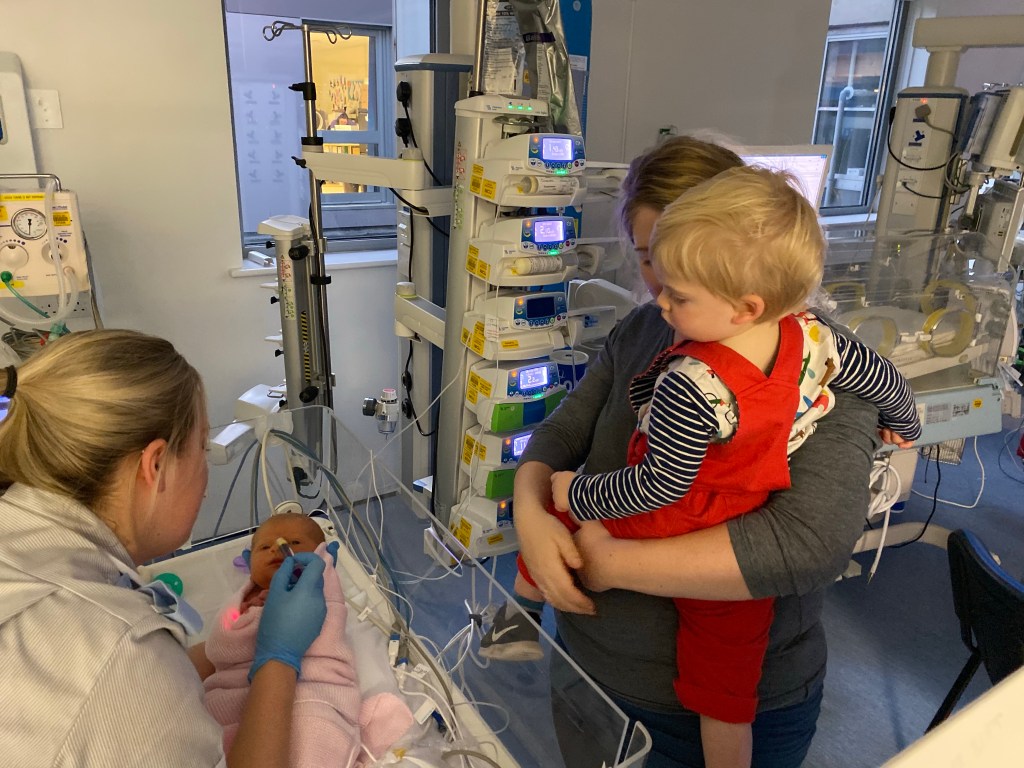
It was a Saturday and Etta had spent 9 days recovering from her first open heart surgery (making her aortic arch bigger and a DORV repair – using a patch to make a tunnel between the left ventricle and aorta). Usually, we would always go straight in to see Etta first thing in the morning because rounds typically started at 8 am. However, today we didn’t. My mum and dad were moving out of their Air BnB in Bristol and driving back to Salisbury for a few days so we went to help them pack up. It was the first time we hadn’t been there for Etta’s morning rounds because we knew we had the whole weekend ahead of us by her bedside because we wouldn’t need to split our time seeing Ezzie. We said goodbye to Ezzie and I went back to Paul’s House (emergency parent accommodation) to express milk before heading over to PICU. Sam went to meet his dad and brother who had come to visit.
I cried a lot as I was pumping milk that morning. I sat on my own in our room thinking how far away this was from what I expected my first few weeks with a second baby would be like. I was so tired of saying goodbye to Ezzie and not having my two babies together and felt incredible guilt for always feeling torn between them.
I met Sam, Tom and Alan at the entrance to the hospital- still crying. I feel a bit of an idiot now for crying so much about saying goodbye to Ezzie, because a few minutes later this would pale into insignificance. As as we arrived onto PICU, we were quickly intercepted by Sophie (one of Etta’s regular nurses). She warned us that something was happening with Etta and there were lots of people around her bed space at the moment.
The NIC (nurse in charge) then came out to speak to us in the only private room we could find- the nurses’ meeting room. She explained that she was just about to call us when we walked into PICU- it was a bit of a coincidence that we had walked in just at that moment. She explained what had happened that morning- Etta had been absolutely fine on morning ward rounds but her nurse Lety had just called the doctors over because her heart arrythmias were getting more and more erratic and sometimes dropping down to 60 beats per minute (it should be 120-160). Her heart rate had been pretty irregular all week which is a common side effect of cardiac surgery because the central part of a heart which contain the messengers for electrical impulses in the heart have been tampered with in surgery and swelling after surgery can also damage it.
When the doctors arrived at Etta’s bed to take a closer look, her heart started dropping further to 40 bpm so they needed to start CPR quickly as she was going into cardiac arrest. The NIC asked if we wanted to come in so we could see what was happening because they could put seats for us nearby. At that moment, we both wanted to be with her but we were terrified about seeing her have CPR. I knew it would be an image we could never erase from our minds (I was right by the way). So I asked the nurse the only question that really mattered:
“Are we going to lose her?”
And the nurse simply replied “I don’t know, I can’t answer that.” This was enough for us- we wanted to be near Etta if these were to be her last moments. Sam’s dad and brother stayed in the meeting room while we went in. There were so many people around her- nurses and doctors administering adrenaline and a nurse giving her chest compressions. The PICU consultant came to tell us what had happened but told us she couldn’t speak for long (because she was still trying to keep Etta alive).
Sam asked if we should call our families- bearing in mind my parents and Ezzie had only left Bristol an hour before. What a difference an hour makes! I still remember the break in his voice as he phoned my mum to tell her that something had happened to Etta and they should come back. Luckily, Sam’s dad had also let the rest of Sam’s family know too. We needed to give everybody the chance to say goodbye to her if she wasn’t going to make it.
I just remember sitting with Sam about 2 metres away from our little girl and the thought “Please don’t die please don’t die please don’t die” running through my mind on repeat.
It was a well-oiled machine around her bed. At the time it was quite intimidating but with hindsight it was very impressive to watch all the staff knowing their different roles and working together. Within 45 minutes Etta seemed to have stabilised. Less and less people were around the bed although the crash trolley was still there just in case.
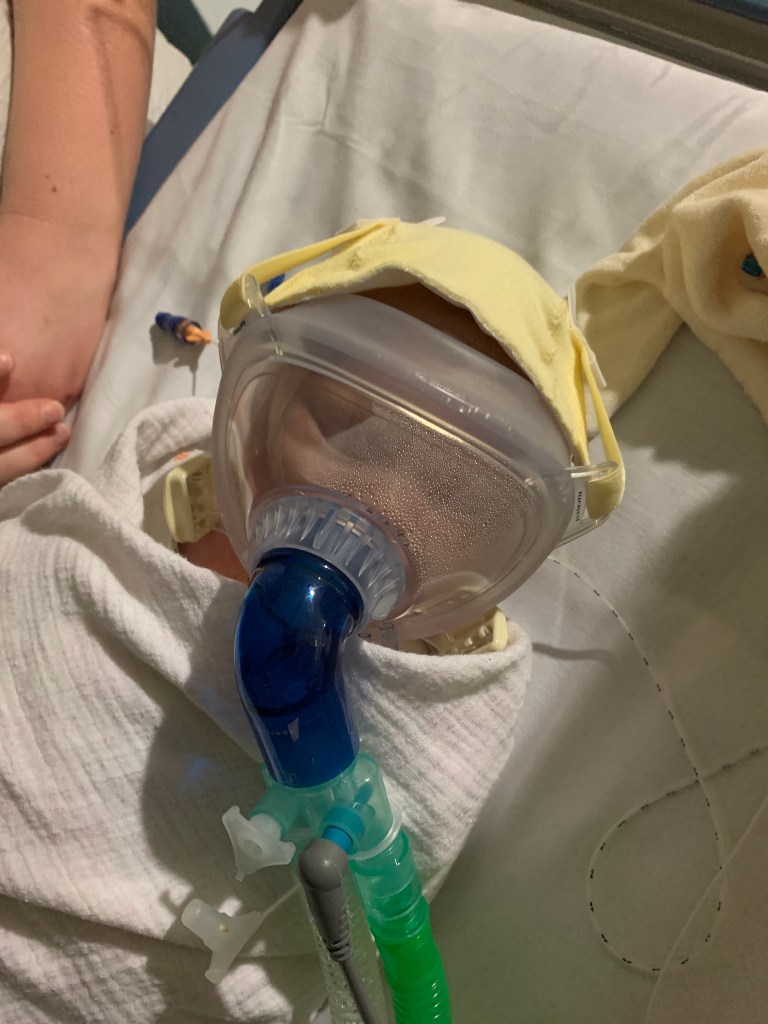
At this point, we were told that she was going to be put on ECMO (which stands for extracorporeal membrane oxygenation) or sometimes called ECLS which is a type of life support where the machine basically acts as your heart and lungs for you outside of your body. We’d been told about it before as very much the ‘last resort’ option if Etta was struggling to cope after her first heart surgery. Survival rates after being put on ECMO for cardiac patients is around 40%. Etta’s chances were possibly higher because she wasn’t completely reliant on this life support yet but it was more being used as a tool to rest her heart before further surgery on Monday. The plan was basically to remove the patch from her previous heart surgery and see if that helped relieve the pressure in her heart.

The intensive care unit was shut down as Etta was put onto ECMO which meant everybody except staff and patients had to leave. This would become a common theme in the next few days with Etta constantly kicking everybody out of PICU. We went into the quiet room with Tom and Alan, as our family started to arrive from different places. My mum and dad had brought Sam’s sister Kim back from Salisbury (leaving Ezzie with Uncle Doug) and my brother Sam and his wife Abi arrived. They hadn’t met Etta yet so I was sad that this was how they were going to see her for the first time. I felt thankful that Sam’s dad managed to meet her the night before.
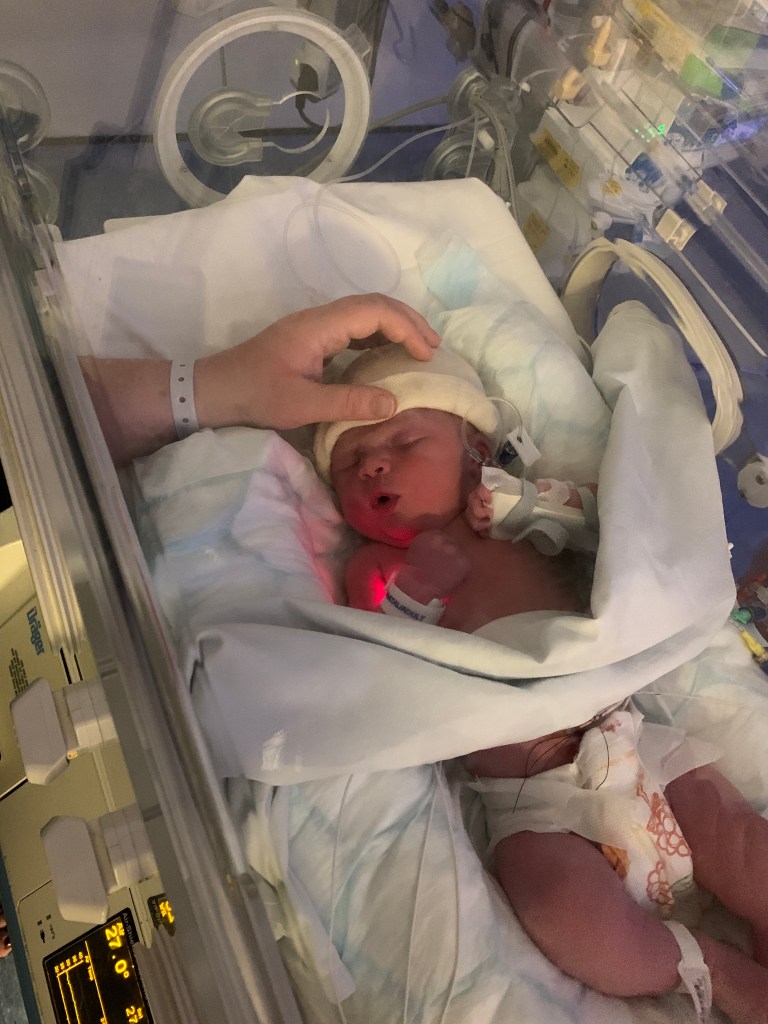
Being in that ‘quiet room’ was hard. We’d seen other families in here over the last few weeks whenever it was bad news. Families gathering to hear progress or say goodbye. And I still couldn’t believe that we were now that family. The day before we’d been having our first cuddles now she didn’t have a breathing tube in and now suddenly we were crowded in this room while Etta was fighting for her life.
If you’re reading this then you’ll know that of course she didn’t die that day. We went back into PICU after an hour or so and Etta had been put onto ECMO. Our family members took it in turns to come and see her 2 at a time- they understood that this visit was precious and could now be their last.
We talked to a perfusionist about the ECMO machine- he had been stolen from the operating theatre because there were no trained ECMO nurses on shift free to monitor the machine. Nobody expected you to need to go onto it- Etta’s nurses were still telling us this the following week when we saw them again. I think it was a shock for everybody.

ECMO is an amazing machine that really can save lives but it is not without its complications. The balance with ECMO is trying to get the correct viscosity of blood- too thin could cause too much bleeding but too thick could cause clots in the circuit which could be very dangerous and stop it from working. While on the ECMO life support, the risks are still high- infections, strokes and brain injury can happen.
The consultants were confident that Etta hadn’t had any prolonged time without oxygen to the brain during her cardiac arrest because they intervened so quickly with CPR. We’ll never actually know. However, because of the ECMO they started monitoring her cerebral activity because it can cause seizures. These would be hard to spot while she was sedated and on muscle relaxants but could be catastrophic if not picked up.
You know it wasn’t a happy ending- despite everybody’s best efforts, Etta still died. Etta had to have a post-mortem after her death which we have not yet received the results of. We are not expecting there to be any big surprises- congenital heart defects causing heart failure and cardiac arrest. My biggest question after her death was ‘Why did she have a cardiac arrest?’ It really felt like it came out of nowhere for us. Her first open heart surgery had a 85-90% success rate and I naively thought once we’d got through that then we would be out of the woods. But we were repeatedly told- ‘we are not out of the woods yet’.
I asked doctors from Bristol Children’s Hospital this question in a meeting after her death to discuss any findings from their internal review. They explained that after surgery, her atrium had dilated and because of her heart arrhythmia this made her very vulnerable to a cardiac arrest. I still don’t understand it all but I’m not a cardiologist so I don’t think I ever will. And as I keep reminding myself , it wouldn’t bring her back anyway. You can quite quickly end up in a dark place if you keep asking ‘what if’ and ‘why’.

This was the scariest day- only the day before we were talking about when she would be moving onto the ward and if we could make it home in time for Christmas or New Year. And then suddenly she was nearly gone in the space of a few minutes. We are so grateful for the nurses and doctors who saved her life that day. We saw the nurse who performed Etta’s chest compressions tirelessly on the day Etta died. We thanked her for saving Etta’s life and giving us extra time with our precious girl.
If she had died from her cardiac arrest, I don’t think I would have recovered from the shock or the guilt of not going in first thing to see her. The truth is if I knew she was going to die (not just that day but ever) then I would have spent even more time by her bedside. But there’s no point dwelling now or blaming ourselves.
We could have lost her in theatre during her first surgery. We could have lost her while we watched on a seat helpless a few metres away. We could have lost her that morning before we’d even had chance to arrive. But we had 9 more days to come to terms with how poorly our little girl really was and to spend time with her before the final goodbye. We lost quite a lot of her that day but we still ended the day with hope that she would get better. And today that hope is different but I still have hope that one day we’ll get to hold her in our arms again.