Well, what a year this week has been! I wasn’t too sure what I wanted to write about this week but with all the talk in the news about CPAP, ventilators and hospital beds, I settled on something I thought was pretty topical at the moment- our experience of intensive care. Etta started her life in NICU (neonatal intensive care) and ended it in PICU (paediatric intensive care) and spent 25 out of 27 days in intensive care (2 were spent in HDU- the high dependency unit on the cardiac ward).
It really saddens me that lots more people are going to be ending up in ICU over the next few weeks and months although hopefully not so many paediatric cases. I know that 25 days is not a long time compared to what lots of families have faced or unfortunately will face but here are a few things I learnt from our time there.

1. Washing your hands really can save lives. The first time we visited NICU was before Etta was born to try and prepare ourselves. You have to leave all coats and bags outside and then get buzzed inside. Then you enter each individual room- we went to look inside ITU 1 (6 cots for the most critical cases) as it was where Etta would be taken. You have to wash your hands by the sink whenever you enter the room and there is sanitiser too. Sam was asked to take his hoody off straight away which I thought seemed a bit overkill at the time but now I get it. In NICU especially, any germs can be life-threatening for these very sick or very premature babies. Soon enough, we were those anxious parents sitting by our baby’s incubator. We then had to take off watches/jewellery and wipe down our phones too. But infections (and viruses as we now know too well) can be deadly and especially so for those in intensive care.
2. You become an expert on a very specific set of medical jargon very quickly. Sam and I were already very aware of the words to describe the heart’s anatomy and Etta’s congenital heart defects (VSD, ASD, coarctation of the aorta, hypoplastic left arch to name but a few) but in intensive care you are also thrown into a world of lots of different machines, acronyms and tests. Suddenly, you can’t help but read all the numbers on the machines and listen into all conversations at your bed space. ‘What was her lactate reading?’, ‘We’ve needed to put her on CPAP’, ‘What was her CRP level?’ It’s pretty relentless. You want to ingest all the possible information about your loved one in case you can help them in anyway. The amazing nurses always took the time to explain every machine and wire to us and answered all our questions. This understanding really helped us feel less anxious- a tiny sense of control in a situation that was very much out of our hands.

3. The camaraderie is like no other I’ve experienced. In a time where parents are living their worst nightmare, smiles are still given freely to others. The parent’s room is where parents can sit down and have a break or anxiously wait if their child is in surgery or the unit is closed for an emergency. You are discussing your worst fears with people you might not even know the names of (although you’ll almost certainly know the name of their child). In PICU, families tended to come and go much more quickly, whilst in NICU, lots of babies stay for weeks or months as they grow bigger. In NICU, the pumping room felt like the eye of a storm- a calm place where you were forced to take a break every few hours and pump breast milk. I will always be very grateful for the kind mums in that room who told me NICU would seem less strange soon, that my milk would come in any day now and how to work the industrial grade breast pump that I was clueless about! It really did feel like a club that no one wanted to be part of but a sisterhood nonetheless. I feel sad that I’ll never know whether all the mums I met made it home safely with their babies and children.
4. Things can change in a matter of minutes, hours or days. I remember the first time we met a family who had been told their child probably wouldn’t survive the night. It was a terrifying prospect- being so close to the edge of death. And then it happened again… and again. A friend I made in NICU, whose baby was quite stable, I met again in PICU a few weeks later because her baby caught an infection and was told she might not make it. And then eventually of course it was us in this touch and go situation. What I realised is that when a baby or child is in intensive care things can go downhill very quickly. The upside to this is that things can get better really quickly too. A week before Etta died, we were called into the ‘quiet room’ to be told that Etta’s life support wasn’t working and that she wouldn’t make it through the night. Then a few hours later, her life support was stable and we were urged to go home and get some rest- she wouldn’t be going anywhere that night. I think you realise quite quickly that life is very fragile in those 4 walls.

5. There’s always someone that is doing better and there is always someone that is doing worse (and it’s all pretty terrible). Life in NICU and PICU was completely humbling. I truly wish I never had to go there but I did and it really opened up to my eyes to the fact we were not unique in having a poorly child. I lost count of the huge range of conditions, illnesses, congenital defects and infections that had brought each child into intensive care- from sepsis to oesophageal atresia and from epilepsy to spinal muscular atrophy. It seems strange now to say that on some days I felt completely lucky that Etta ‘only’ had a heart condition that could be fixed with surgery and we would get to take her home relatively healthy. We met families whose children had lifelong disabilities so would be in and out of PICU throughout their life or had life-limiting conditions which meant they would soon die in hospice care.
I also felt incredibly lucky when families were blue lighted in with their baby’s life hanging by a thread while Etta was stable in her cot and recovering from her planned surgery. And on the other side of the fence, it’s true that I felt jealous too when many families were able to move onto the wards, back to local hospitals or even better- home. We saw lots of babies come and go with RSV and bronchitis and I really wish that was all Etta had to deal with. But the truth is if your child is in intensive care for days, weeks or months- it’s all horrendous and I really wish no one had to go through it.
A few times we were that family who were doing worse. Screens were pulled round (that’s when you know it’s serious), extended family members were taking it in turns to spend time with Etta and there were many sympathetic looks from parents walking past, thanking god it wasn’t their child today. There is nothing like intensive care to make you realise how precious life really is- it’s a platitude but it’s also the truth.

6. The NHS is amazing. We know this already- of course we do. That’s why millions of people stood on their doorsteps to clap this week. But I think until they’ve saved you or a family member’s life you don’t realise quite how lucky we are in England. In Etta’s short life she was looked after by: cardiologists, obstetricians, midwives, intensivists, paediatricians, NICU and PICU nurses, cardiac nurses, physiotherapists, dieticians, pharmacists, maternity care assistants, health care assistants, sonographers, radiographers, anaesthetists, perfusionists, NEST drivers, cardiac surgeons, porters and I’m sure even more that I wasn’t aware of. She had incredible care by incredible staff- and we didn’t even pay a penny for it. It was hard to hear when people were complaining about the staff or not being able to come into PICU when a procedure was going on and lots of other little grumbles. They truly went above and beyond to try and save our little girl and we know that her nurses and doctors in particular were really hurting alongside us when they couldn’t. I know that Etta’s care would have cost tens of thousands of pounds but really the tenderness that was shown to her and our family by all of the NHS was truly priceless. We will never be able to repay them.
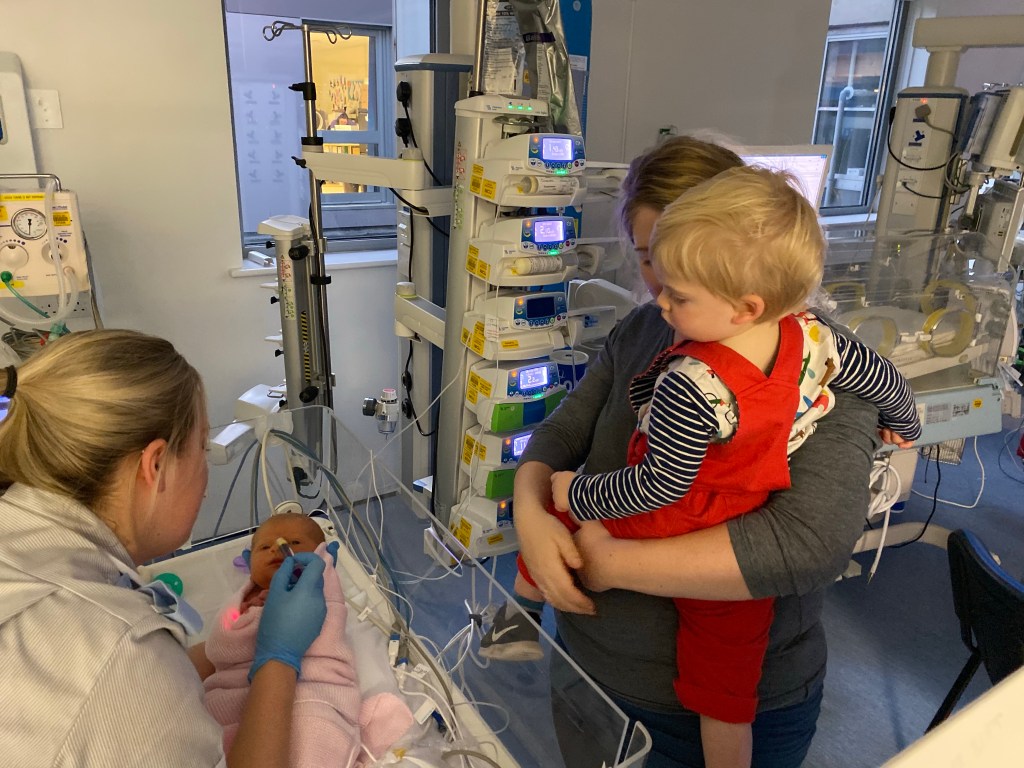
I wish that nobody had to go through having a loved one in intensive care. But for those that do I hope that they can at least come out of the other side with a new appreciation for life, the NHS or each other.
Hi dear Emm and Sam. Again so beautifully written. In the picture, Etta really looks like you both and she seems to have a deep knowledge and understanding resonating from her. Thinking of Etta and you all. Mandy Xxx
LikeLike
Beautifully written once again Emily; each of your’s and Sam’s blogs are brave, insightful, inspirational and humbling. x
LikeLike
Thank you for your blog. Currently 37 weeks preganat with our first baby who has hlhs xx
LikeLiked by 1 person